Brochure
Please complete the form below and we will send you our brochure
Contact

The defense industry faces global challenges as it advances into the next decade of land, air and sea protection. From developing technology to brand-new business models, the market in France, Europe and the U.S. will stand witness to many interesting growth trends and increased investment amid an increasingly complicated geopolitical landscape.
The United States is expected to spend $115 billion annually on advanced air mobility alone by 2035. France, one of the leaders in global defense spending, maintains an annual military budget of $47.9 billion. Military spending in Europe reached $356 billion in 2019 and the region is seeking to gain strategic autonomy by 2025.
However, multiple setbacks, including the pandemic spending and a possible recession, might require these regions to look for cost savings solutions. Europe already faces coordination issues, with EU states showing preferences in investing domestically, often to the detriment of the different states’ ability to achieve a cohesive weapon and defense system.
France will face growth challenges in new arenas, including cyber defense and outer space. Futuristic concepts such as quantum technology, artificial intelligence systems and directed energy weapons will receive $1 billion in investments from the government and the country will also need to divert funds into infrastructure and maintenance to upkeep existing military equipment and capabilities.
The U.S., France and the whole of Europe will still move forward with solid investment in military personnel and their health. These armies, navies and air forces, needing to be efficient and cost conscious, will need to seek solutions that will support operators in the field, reducing stress points and bolstering physical and mental health.
Stress, both physical and psychological, takes a toll on service men and women in the field and on bases across the globe –– oftentimes more taxing on the generals and officers who have to make critical decisions under extremely delicate situations. Combatants in the field, specifically, encounter numerous physical stressors in relation to their own personal protective equipment (PPE). The weight, mobility and comfort of PPE hasn’t been prioritized in the past, but militaries are now realizing the critical importance of reducing stress points in this area.
Military leaders know that a mobile soldier is a survivable soldier. In that respect, militaries, like in the U.S., are investing heavily in lightweight wearables to make combat gear less burdensome. From new modular vests to lighter ceramic plates, wearables provide combatants with better mobility and less physical stress on the field. Sensors in these high-tech wearables can also track soldier’s health status in real time, allowing operators to retreat members whose physician conditions are at risk and adjust the intensity level of military training based on physiological indicators as monitored by smart wearables.
But physical stressors aren’t the only major health risk confronting our armed forces. Military leaders are also recognizing the toll of emotional strain on our service men and women, not to mention the PTSD epidemic among veterans and wounded soldiers.
Separated from their families while working in hazardous environments with extraordinary physical demands, “enlisted military” is ranked as the world’s most stressful job field. Unchecked emotional stress can often lead to potentially major health risks that can compromise not just soldiers’ health status, but also mission-critical operations. But any technology that can support these service individuals must be cost efficient, not weigh down field operators nor expose them to dangers by connecting to bluetooth technology.
And stress and health issues don’t remain on the battlefield. While many of the emotional impacts of military life can be invisible to the eye, they have a very physical impact on the body. Among veterans who served in active combat, 17% reported symptoms of PTSD. The healing and treatment of wounded soldiers and veterans, as PTSD is often associated with medical conditions such as cardiovascular disease, asthma, chronic pain and diabetes.
In order to grow revenue in a competitive environment, companies that service military customers should consider building products that offer value-added capabilities to traditional PPE. These firms may find an edge by incorporating lightweight and wearable technologies to existing military gear. Competition in the space is fierce, and companies that move quickly into emerging technologies will likely be rewarded with large contracts.
It is incumbent on militaries to invest in veteran care in the most cost effective way possible. If such approaches are invested in early and strategically, responsible governments will see compelling results. Companies that bid on military contracts will see huge benefits if they move quickly into making products that service these needs.
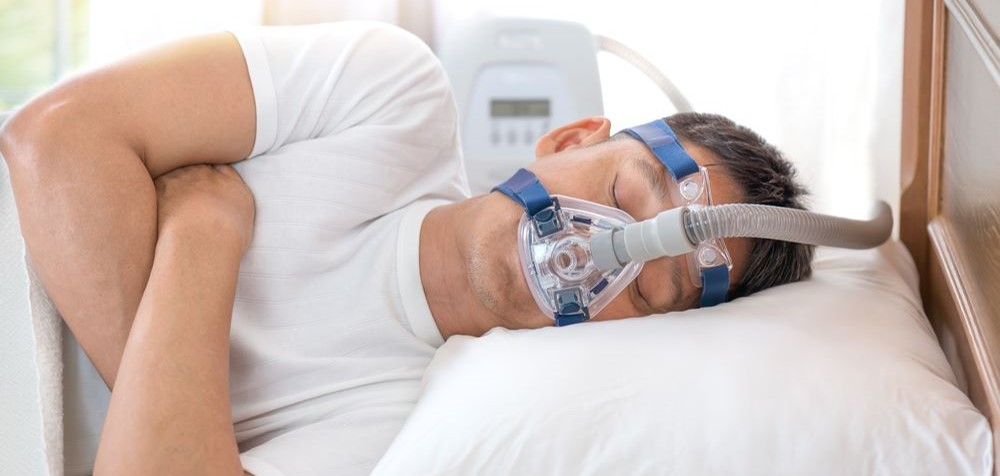
Sleep apnea is a chronic condition that is often underdiagnosed, impacting the quality of life and presenting secondary risks. In France, approximately 5% of the adult population is affected. The primary treatment relies on nocturnal positive airway pressure ventilation (CPAP). The main challenge lies in ensuring compliance with this treatment, as it is crucial for its effectiveness. However, despite significant technical advancements, this device is still poorly accepted and tolerated by patients. Telemonitoring represents a complementary solution that can significantly enhance sleep apnea treatment.
Obstructive sleep apnea syndrome (OSAS) involves repeated episodes of airway obstruction in the upper respiratory tract, leading to breathing pauses. Complete blockage results in apneas, while partial blockage leads to hypopneas.
Loud snoring, restless and non-restorative sleep, and daytime sleepiness are common signs that suggest a diagnosis. Fatigue upon awakening affects the overall well-being, both physically and mentally, with an impact on social life.
However, the link between these symptoms and the possibility of OSAS is not always recognized, leading to a significant rate of underdiagnosis.
In addition to significantly affecting the quality of life, untreated and severe sleep apnea exposes patients to various health consequences:
To establish a diagnosis and provide appropriate treatment, additional tests are necessary. Home-based polygraphy records respiratory parameters during the night. This telemonitoring system serves as a preliminary diagnostic examination, facilitating the screening of OSAS.
Polysomnography, also known as sleep recording, is a more comprehensive examination that analyzes sleep patterns along with respiration. It can be performed at home or in a healthcare facility, confirming the diagnosis and providing detailed information on its severity.
Continuous positive airway pressure (CPAP) therapy is currently the only proven treatment for severe OSAS. By keeping the upper airways open, this treatment reduces the number of apneas and hypopneas. Its effectiveness has been demonstrated in numerous studies.
The patient’s adherence to CPAP treatment determines its effectiveness. Therefore, the choice of respiratory assistance device, selection of the most suitable mask, adjustment of device parameters, etc., are all crucial aspects. The healthcare provider plays a crucial role in the treatment’s implementation, which requires a period of 1 to 2 weeks for adaptation. Initially, it is essential to verify the correct and regular use of the CPAP device at home. Telemonitoring allows data transmission to the healthcare provider for better adjustment.
Regarding lifestyle, patients should be encouraged to lose weight as obesity and overweight are aggravating factors. Other factors that contribute to sleep apnea include alcohol consumption and sedative use. In cases of mild to moderate sleep apnea, mandibular advancement devices (MAD) can be tried as a priority.
Respiratory devices can be noisy and cumbersome for patients, potentially causing discomfort for both the patient and their partner. Patients often make an initial effort but become discouraged by what they perceive as a complex and restrictive device, resulting in low compliance or discontinuation of its use.
When compliance is insufficient, it is crucial to identify the reasons, which can vary significantly.
Therapeutic education is now a fundamental aspect of managing chronic diseases. Active patient involvement in their treatment is a key component of successful management.
A few years ago, a participatory consultation involving professionals (doctors, manufacturers, healthcare providers), and patients led to proposals aimed at improving the follow-up and support of patients with sleep apnea. Among the suggested solutions to improve treatment adherence, telemonitoring offers positive aspects.
Furthermore, while improving the patient’s health remains the central objective, cost containment in the context of sleep apnea is also crucial.
The complexity of managing OSAS has led to the consideration of telemonitoring as a tool to support and encourage patients to comply with their treatment.
Since early 2018, telemedicine has been regulated for sleep apnea syndrome, requiring the involvement of a physician. Telemonitoring complements the ongoing care and the doctor-patient relationship without replacing follow-up consultations.
Chronolife positions itself as an expert partner in remote medical monitoring for sleep apnea treatment. Through direct respiratory rate monitoring, it becomes possible to demonstrate to non-compliant patients that the number of apneas is higher, thereby motivating them to reinitiate treatment.
In addition to providing information on compliance, telemonitoring provides physicians with data to measure treatment effectiveness through indicators such as leaks, pressures, and residual apnea-hypopnea index (AHI). Telemonitoring complements the patient’s medical record, allowing for fine-tuning of parameters if necessary, ensuring tolerance, and addressing any adverse effects.
Ultimately, this additional information helps in more effectively assessing the balance between benefits and risks and the satisfaction of the patient’s needs.
The management of OSAS is crucial due to its potential impact on the apneic patient. In a strengthened relationship of trust, telemonitoring allows patients and physicians to adjust the treatment together.
REFERENCES:
The Keesense solution, manufactured by Chronolife, is designed for continuous monitoring of physiological parameters. Version 1 of this medical device is a regulated healthcare product and carries the CE mark (in accordance with European Directive 92/43/EC). Please read the instructions for use carefully. Keesense version 2 is undergoing certification according to the requirements of the new medical device regulation (2017/745/EU). July 2023.
The combined effects of an aging population and the increasing incidence of chronic diseases are leading to more hospital admissions. This situation is increasing the pressure on already overburdened care facilities. The challenge for hospital systems is to avoid service overcrowding – especially in the current pandemic context -, without sacrificing the care of their patients. How to relieve the hospitals while ensuring patient follow-up? Here are some answers.
Leading cause of death in the world according to the WHO, chronic diseases are responsible for 63% of deaths. Heart failure, diabetes, COPD, cancer… the management of these pathologies must be carefully reviewed, with the aim to better the patient’s quality of life, through an adapted continuum of care.
Nowadays, the therapeutic follow-up of most patients with chronic diseases aims to maintain a stable condition, through drug and surgical treatments, but also through prevention advice to encourage a healthier lifestyle. Care is provided during periodic consultations throughout the year and during hospitalizations, which are often too numerous. For several chronic pathologies such as heart failure, respiratory failure or even cancer, these hospitalizations are often associated with increased morbidity and mortality.
In the next 40 years, the number of people above the age of 65 in the European Union is expected to double, increasing from 85 million in 2008 to 151 million in 2060. Considering the fact that this population consumes more care and that it often experiences chronic diseases, its care constitutes a challenge for hospitals. The issue at stake is to implement more precise and personalized long-term monitoring systems to manage patients at home, and only admit to hospital those who really need it.
Readmissions are taking a toll on national health budgets, which are already under pressure due to increasing demands and rising healthcare costs, a situation that is expected to worsen in the upcoming years. The development of ambulatory surgery and the shortening of the average length of stay are part of the measures implemented, but they will require increasingly precise home monitoring.
Ultimately, hospitals should be able to limit readmissions and maintain sick people at home by guaranteeing them a high-quality follow-up, to avoid a saturation of the care system. In France, a study conducted on 1,000 patients aged 75 and over admitted in nine hospitals in an emergency, showed that 14.2% of patients had to be readmitted within 30 days, unexpectedly. Implementation of procedures ensuring patient mobility and independence in the 24 hours following surgery, clear communication with patients, close monitoring of their health status in the two weeks following their discharge from the hospital… Several factors have been identified to anticipate health deterioration and avoid re-hospitalization.
Monitoring patients by implementing new home health devices can help avoid unnecessary (re)hospitalizations. Remote patient monitoring is an effective response to this issue as it allows healthcare professionals to monitor patients remotely, by having access to physiological data in quasi-real time. Reducing office visits, anticipating worsening of the patient’s health status, making early diagnosis, improving the patient’s quality of life by ensuring a real continuity of care… all are advantages guaranteed by the implementation of a remote monitoring system.
To be truly useful to healthcare professionals, without constituting an additional workload, it is preferable that remote monitoring be based on a multiparametric device, supported by a comprehensive service providing complete care. This kind of solution allows the remote surveillance of patient’s physiological variations, without impacting their quality of life. Electrocardiogram, respiration, temperature, pulmonary impedance… recent technological breakthroughs make it possible to equip medical devices with multiple sensors, providing healthcare professionals with relevant data for diagnosis. In the long term, chronic conditions could benefit from a more personalized, regular, and accessible monitoring.
Aware of the necessity to relieve hospitals while guaranteeing an efficient monitoring of patients, Chronolife has developed a connected smart t-shirt, able to continuously collect 6 physiological parameters, throughout the patient’s daily life. Machine washable and easily “forgotten” by patients, this medical device is easy to wear and constitutes a reliable tool to implement remote monitoring.
Eventually, the adoption of such solutions by care systems should lead to a better management of patients with chronic diseases and secure homecare for sick and frail people, ensuring a continuum of care between hospital and home.
One example of the collateral consequences of the Covid-19 pandemic is that patients suffering from chronic pathologies have been avoiding hospital consultations since March 2020. Out of fear of being contaminated, but also on the recommendations of the health authorities, they preferred to postpone or simply cancel their appointments, causing health professionals to fear a delay in treatment and a potentially serious risk of decompensation. Under such context, the widespread use of teleconsultation and telemonitoring has never been more relevant. Explanations.
At risk for serious medical complications, some chronically ill patients were encouraged to be more cautious with Covid and to stay at home as much as possible. For these patients, periods of confinement presented a real risk: many cancelled their routine follow-up appointments. A false good idea, which health professionals tried to warn about as early as the end of March.
Moreover, the increase in sedentary lifestyle can have consequences on the exacerbation of several pathologies such as depression, obesity, etc.
Everything from implementing separate circuits between suspect patients and non Covid-19 patients, disinfecting premises and equipment, personalizing support methods, to providing automatically renewed prescriptions, several actions have been undertaken to reassure the chronically ill and make them return to hospitals, albeit without always meeting with success. At the same time, doctors have proposed teleconsultation. “For a patient with heart failure, for example, we can simply ask them to weigh themselves at home and ask them if they experience shortness of breath when they climb the stairs. This is one of the signs that will lead us to suggest that they come and see us, while putting protective measures in place,” explained Pierre-Louis Druais, a general practitioner and member of the scientific council, on BFMTV in April.
Teleconsultation has therefore established itself as a safe way to keep in touch with patients, but simple bathroom scales quickly reach their limits when it comes to providing a positive patient experience and serving as viable diagnostic tools. With devices such as connected scales offering limited visibility into patients’ health status, remote monitoring devices allowing continuous multi-parameter monitoring has thus proven to be particularly suitable.
Preventable hospitalization, easier home care, improved medical follow-up, and early detection of a deterioration in health status for appropriate medical decision making… These are just some of the prime examples of the great promise of remote monitoring for patients with diabetes, COPD, sleep apnea and heart failure. In this new paradigm, patients can continue to live normally at home, knowing that their health status is being monitored. But for telemonitoring to really work, it is necessary to rely on medical devices that are reliable, comfortable and ergonomic for the patient, who must be able to live a normal life, forgetting that they are telemonitored. A new range of lighter, more reliable medical devices is emerging with new embedded technologies, all with the objective of better monitoring and greater acceptability by patients.
Last but not least, these tools must be offered to healthcare professionals to help them better monitor their patients without burdening them with additional work, i.e. generating untimely alerts or false alarms…
Aware of these issues, Chronolife has developed a patented intelligent t-shirt, capable of continuously capturing 6 different physiological parameters in real life :
Unlike other telemonitoring solutions, Chronolife integrates the sensors directly into the fabric, so patients can wear the shirt like any other garment and machine wash it. This ease of use improves compliance and paves the way for continuous remote monitoring. Thanks to Chronolife, healthcare professionals have accurate information on the health status of their patients, without the need to have them travel to the hospital. This reliable diagnostic tool enables them to fully ensure the continuity of care between the hospital and the patient’s home, and avoid any risk of contamination to these fragile populations.
Monoclonal antibodies, stem cells, biotech, messenger RNA vaccines: over the last 10 years, advances in life sciences have led to exciting therapeutic innovations. The unprecedented alliance of genetics, data, imaging, and robotics is contributing to the emergence of ever more agile innovation ecosystems, grouped under the same objective: provide patients with new methods of diagnosis and effective treatments. While the role of the pharmaceutical industry remains crucial in this new paradigm, it must also reinvent itself to remain competitive and in tune with the needs of doctors as well as the ones of their patients. Continuum of care, prevention, personalization of healthcare offers and differentiation strategies: it is by using products and services developed by the new e-health players that the pharma and life sciences industry can effectively meet the challenges implied by a more efficient or a more complex and connected healthcare world.
More and more, patients will have to be cared for outside hospital walls. Therapeutic effectiveness and compliance programs that were traditionally “controllable and monitored” by health care institutions during hospital stays will become less common. In this context, with shorter hospital stays and patients constantly on the move, pharmaceutical groups will want to have real-life data on patients to better assess the therapeutic effectiveness of their treatment, particularly when it will come to price negotiations. Connected and digital healthcare tools adapted to each therapy and use case can optimize the continuum of patient care between healthcare establishments, cities, and patients’ homes. It really appears as an additional opportunity for laboratories to strengthen their connections with the various stakeholders around the patient.
The expiration of patents and the rise of generic medication will lead pharmaceutical companies to offer new services around medication to strengthen their relationship with healthcare professionals. By focusing only on medication, it will be difficult for a laboratory to distinguish itself from others. The solution lies in “beyond the pill”, in other words it lies in the ability to take advantage of new technologies to offer new services that go beyond basic medication. Several laboratories have therefore understood this specific issue by creating their own entity to develop e-health solutions, or by forming partnerships with IT companies.
To gain efficiency and to create value, laboratories will have to increasingly become part of the inevitable development of e-health and the opportunities that go with it: medication, medical devices, connected devices, or even healthcare applications. One of the best ways to create value is to offer healthcare solutions that combine products and services. In this way, laboratories will be able to:
In this new value chain, all the products and services that are offered are designed accordingly to the customer journey of each of the players implied in the medication industry, with benefits designed for the long term. Personalizing the healthcare offer by combining products and services is a real opportunity for laboratories to provide a global service to practitioners, and to create a new relationship between them and the pharmaceutical companies as well.
Chronic diseases represent an annual cost of 115 billion euros to the countries of the European Union, or 0.8% of GDP. Given the aging of the population, it is inevitably a major challenge. In this context, it is not surprising that health authorities are increasingly insisting on the importance of prevention, which could save several billion euros every year in Europe. Even though the Social Security budget allocated to prevention has remained unchanged for 15 years, but that is another story.
Completely in line with actual predictive, preventive, and personalized healthcare, which is organized around evidence and care pathways, many innovative players are now offering patients a better understanding of their state of health. This paradigm shift requires laboratories to diversify their portfolio, by including more therapeutic education, telemonitoring and prediction for patients with chronic pathologies to limit or to anticipate any kind of recurrences. Here again, digital technology represents a crucial source of help for laboratories. As part of what could be called a more “around the pill” approach, it can be used to improve the effectiveness of medication by setting up associated services. As part of this strategy, digital technology will make it possible to find additional sources of revenue apart from using medication itself.
Thanks to its expertise in the integration of sensors on wearables, Chronolife has come up with a portfolio of patented technological tools, enabling laboratories to offer a new generation of medical devices that meet health and safety certifications. These solutions allow the pharmaceutical industry to position itself on a differentiating service offer, to be one step ahead of the competition, and of course in compliance with security protocols with respect to patient data.
In the world of insurance, acquiring new customers is expensive and retaining customers is increasingly difficult. The cost of acquiring a new customer is estimated between 700 and 800 euros. Whereas only a few years ago, an insurer could expect to keep a client for about 9 years, now the average is down to 4 years. These challenges are exacerbated by the implementation of the Hamon Law, which allows insured individuals to cancel their contracts at any time after one year. Not to mention that, for loans and mortgages, borrowers no longer have the obligation to take out a policy with the lenders’ arranged insurer… It is under this context that insurers have every interest in differentiating themselves by offering new, useful and innovative services to their insured, in order to increase customer loyalty. Prevention and risk reduction actions – beyond simple health education – thus represent tremendous opportunities for insurers and mutuals, both for individual and group insurances. Explanations:
A few years ago, many insurance companies and mutual insurance companies began to engage in so-called “health education” prevention, i.e. the implementation of prevention programs to encourage their policyholders to adopt new, healthier behaviors. While the intention was good, the impact of these initiatives remained very limited. For the consumers and companies, we need to be able to go further beyond prevention by proactively anticipating risk factors, which can support people in safely returning to work, reduce accidents or to limit re-hospitalization in the event of chronic illnesses.
One example among others: setting up a remote patient monitoring platform for policyholders suffering from chronic heart failure or respiratory insufficiency. Beyond offering an innovative and useful solution, this kind of risk prevention program has the advantage of recreating a connection with policyholders.
To achieve this, you need to be able to rely on connected healthcare devices that go beyond simple coaching actions. Ordinary connected bracelets and other step counters are not adequate; the selected device must be able to anticipate the deterioration of the state of health like the Chronolife connected t-shirt. Easy-to-use and machine washable like any other t-shirt, this solution offers continuous monitoring of wearers’ real life situations in a comprehensive manner, on 6 different physiological parameters: electrocardiogram, thoracic and abdominal respiration, physical activity, skin temperature and pulmonary impedance.
Offering a solution such as Chronolife is also an opportunity for the insurer to forge deeper connections with the insured, and bring value to important subjects such as the policyholders’ health conditions, apart from the premium calls and claims management.
On the business side, the insurer can provide tools to monitor people at risk, according to their unique financial and strategic conditions. Thus, offering a platform of prevention services, combined with a remote monitoring solution, will be particularly valuable for vulnerable workers, isolated workers and workers with risk factors. Several possibilities are available to the insurer:
Offering a device such as Chronolife in your business services offer will help to increase the loyalty of these key accounts. Solutions like this will also help you provide value-add, complementary services that will differentiate your insurance offering beyond price, and help you win calls for tenders.
Increasingly committed to CSR policies, companies are indeed interested in developing effective prevention actions for their employees for specific health conditions and wellness requests. Offering such a service makes it possible to respond to increasingly pressing demand from companies, while standing out from other players. Several pricing models are possible, ranging from more or less shared care between mutual insurance companies and remote monitoring providers, to some levels of investment by the end user / policy holder. Are you interested? Contact us to tell us about your needs and how we can help take your insurance business offering to the next level!
| Cookie | Duration | Description |
|---|---|---|
| cookielawinfo-checkbox-analytics | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Analytics". |
| cookielawinfo-checkbox-functional | 11 months | The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". |
| cookielawinfo-checkbox-necessary | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookies is used to store the user consent for the cookies in the category "Necessary". |
| cookielawinfo-checkbox-others | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Other. |
| cookielawinfo-checkbox-performance | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Performance". |
| viewed_cookie_policy | 11 months | The cookie is set by the GDPR Cookie Consent plugin and is used to store whether or not user has consented to the use of cookies. It does not store any personal data. |
