The Next Digitization Frontier for the Defense Industry: Remote Health Monitoring
The Next Digitization Frontier for the Defense Industry: Remote Health Monitoring Global Investments On the Rise to Modernize Defense …
Brochure
Please complete the form below and we will send you our brochure
Contact
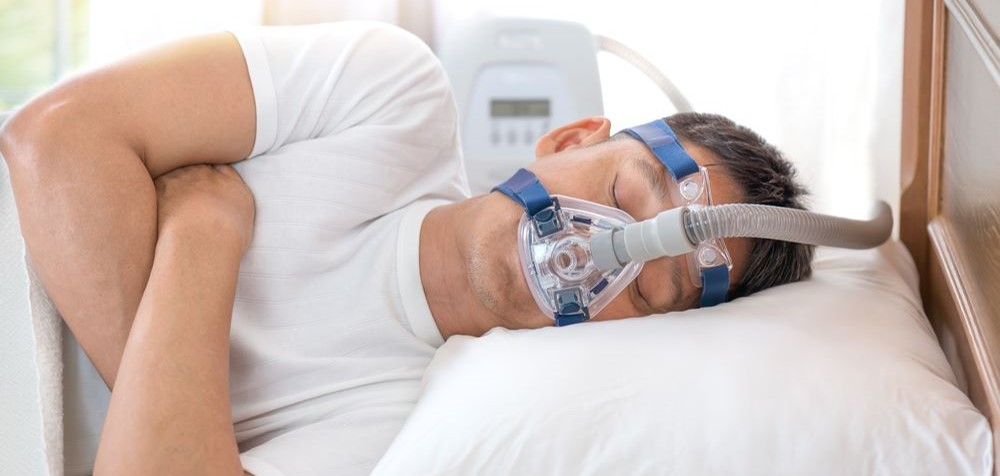
Sleep apnea is a chronic condition that is often underdiagnosed, impacting the quality of life and presenting secondary risks. In France, approximately 5% of the adult population is affected. The primary treatment relies on nocturnal positive airway pressure ventilation (CPAP). The main challenge lies in ensuring compliance with this treatment, as it is crucial for its effectiveness. However, despite significant technical advancements, this device is still poorly accepted and tolerated by patients. Telemonitoring represents a complementary solution that can significantly enhance sleep apnea treatment.
Obstructive sleep apnea syndrome (OSAS) involves repeated episodes of airway obstruction in the upper respiratory tract, leading to breathing pauses. Complete blockage results in apneas, while partial blockage leads to hypopneas.
Loud snoring, restless and non-restorative sleep, and daytime sleepiness are common signs that suggest a diagnosis. Fatigue upon awakening affects the overall well-being, both physically and mentally, with an impact on social life.
However, the link between these symptoms and the possibility of OSAS is not always recognized, leading to a significant rate of underdiagnosis.
In addition to significantly affecting the quality of life, untreated and severe sleep apnea exposes patients to various health consequences:
To establish a diagnosis and provide appropriate treatment, additional tests are necessary. Home-based polygraphy records respiratory parameters during the night. This telemonitoring system serves as a preliminary diagnostic examination, facilitating the screening of OSAS.
Polysomnography, also known as sleep recording, is a more comprehensive examination that analyzes sleep patterns along with respiration. It can be performed at home or in a healthcare facility, confirming the diagnosis and providing detailed information on its severity.
Continuous positive airway pressure (CPAP) therapy is currently the only proven treatment for severe OSAS. By keeping the upper airways open, this treatment reduces the number of apneas and hypopneas. Its effectiveness has been demonstrated in numerous studies.
The patient’s adherence to CPAP treatment determines its effectiveness. Therefore, the choice of respiratory assistance device, selection of the most suitable mask, adjustment of device parameters, etc., are all crucial aspects. The healthcare provider plays a crucial role in the treatment’s implementation, which requires a period of 1 to 2 weeks for adaptation. Initially, it is essential to verify the correct and regular use of the CPAP device at home. Telemonitoring allows data transmission to the healthcare provider for better adjustment.
Regarding lifestyle, patients should be encouraged to lose weight as obesity and overweight are aggravating factors. Other factors that contribute to sleep apnea include alcohol consumption and sedative use. In cases of mild to moderate sleep apnea, mandibular advancement devices (MAD) can be tried as a priority.
Respiratory devices can be noisy and cumbersome for patients, potentially causing discomfort for both the patient and their partner. Patients often make an initial effort but become discouraged by what they perceive as a complex and restrictive device, resulting in low compliance or discontinuation of its use.
When compliance is insufficient, it is crucial to identify the reasons, which can vary significantly.
Therapeutic education is now a fundamental aspect of managing chronic diseases. Active patient involvement in their treatment is a key component of successful management.
A few years ago, a participatory consultation involving professionals (doctors, manufacturers, healthcare providers), and patients led to proposals aimed at improving the follow-up and support of patients with sleep apnea. Among the suggested solutions to improve treatment adherence, telemonitoring offers positive aspects.
Furthermore, while improving the patient’s health remains the central objective, cost containment in the context of sleep apnea is also crucial.
The complexity of managing OSAS has led to the consideration of telemonitoring as a tool to support and encourage patients to comply with their treatment.
Since early 2018, telemedicine has been regulated for sleep apnea syndrome, requiring the involvement of a physician. Telemonitoring complements the ongoing care and the doctor-patient relationship without replacing follow-up consultations.
Chronolife positions itself as an expert partner in remote medical monitoring for sleep apnea treatment. Through direct respiratory rate monitoring, it becomes possible to demonstrate to non-compliant patients that the number of apneas is higher, thereby motivating them to reinitiate treatment.
In addition to providing information on compliance, telemonitoring provides physicians with data to measure treatment effectiveness through indicators such as leaks, pressures, and residual apnea-hypopnea index (AHI). Telemonitoring complements the patient’s medical record, allowing for fine-tuning of parameters if necessary, ensuring tolerance, and addressing any adverse effects.
Ultimately, this additional information helps in more effectively assessing the balance between benefits and risks and the satisfaction of the patient’s needs.
The management of OSAS is crucial due to its potential impact on the apneic patient. In a strengthened relationship of trust, telemonitoring allows patients and physicians to adjust the treatment together.
REFERENCES:
The Keesense solution, manufactured by Chronolife, is designed for continuous monitoring of physiological parameters. Version 1 of this medical device is a regulated healthcare product and carries the CE mark (in accordance with European Directive 92/43/EC). Please read the instructions for use carefully. Keesense version 2 is undergoing certification according to the requirements of the new medical device regulation (2017/745/EU). July 2023.
The Next Digitization Frontier for the Defense Industry: Remote Health Monitoring Global Investments On the Rise to Modernize Defense …
The combined effects of an aging population and the increasing incidence of chronic diseases are leading to more hospital admissions.…
One example of the collateral consequences of the Covid-19 pandemic is that patients suffering from chronic pathologies have been avoiding…
Monoclonal antibodies, stem cells, biotech, messenger RNA vaccines: over the last 10 years, advances in life sciences have led to…
In the world of insurance, acquiring new customers is expensive and retaining customers is increasingly difficult. The cost of acquiring…
| Cookie | Duration | Description |
|---|---|---|
| cookielawinfo-checkbox-analytics | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Analytics". |
| cookielawinfo-checkbox-functional | 11 months | The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". |
| cookielawinfo-checkbox-necessary | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookies is used to store the user consent for the cookies in the category "Necessary". |
| cookielawinfo-checkbox-others | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Other. |
| cookielawinfo-checkbox-performance | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Performance". |
| viewed_cookie_policy | 11 months | The cookie is set by the GDPR Cookie Consent plugin and is used to store whether or not user has consented to the use of cookies. It does not store any personal data. |
